 Professor of surgery J. Calvin Coffey is refuting a century’s worthy of knowledge about abdominal anatomy, claiming it is wrong and remapping the human mesentery as has never been done before. If proven correct, the research led by the Graduate Entry Medical School at UL Colorectal Surgeon may change the treatment of inflammatory bowel diseases, leading to less invasive surgeries, fewer complications, faster patient recovery, and lower overall costs.
Professor of surgery J. Calvin Coffey is refuting a century’s worthy of knowledge about abdominal anatomy, claiming it is wrong and remapping the human mesentery as has never been done before. If proven correct, the research led by the Graduate Entry Medical School at UL Colorectal Surgeon may change the treatment of inflammatory bowel diseases, leading to less invasive surgeries, fewer complications, faster patient recovery, and lower overall costs.
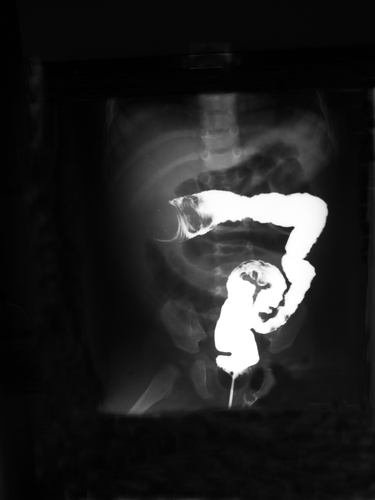
“The blood vessels which supply the gastrointestinal tract (gut) travel through the mesentery — a structure which attaches the intestine to the abdominal walls, and holds it in place and defends against the spread of disease, including cancer,” explained Coffey. “However, for over 100 years the anatomy of the mesentery has been incorrectly described. Our research has found that this critical part of abdominal anatomy is a simpler structure than previously thought, and this is having a major impact across all related scientific and clinical disciplines.”
Coffey conducted a series of combined multiple investigations, using tools such as 3D imaging, in order to fully map the anatomical structure of the mesentery correctly, in partnership with Professor Peter Dochery and Dr Fabio Qunadematteo (NUIG), and Professor Colum Dunne (GEMS/UL). Their research was already published in the Annals of Surgery journal, the Journal of Anatomy, The Surgeon, Colorectal Disease, as well as other reference medical journals.
“Inaccurate understanding of structure has greatly hampered our understanding of this organ. Increasingly we are recognizing that the mesentery plays a crucial role in controlling metabolic, immunologic and endocrine functions such that it is now regarded as a driver of disease processes including diabetes mellitus, ischaemic heart disease, and peripheral vascular disease,” said Coffey.
The recent clarification of mesenteric organ structure will greatly aid pathologists in understanding gastrointestinal diseases, radiologists in interpreting the appearance of abdominal diseases in general, and surgeons in anatomically correcting these diseases. By following these findings, surgeons can now perform abdominal surgery with minimal complications, and “trainee surgeons can be trained to perform it in a reproducible manner that heretofore was not possible,” he added.
The findings of the research may have implications in the treatment of diseases of the bowel, especially regarding the identification of new biological markers that may be used in oncological cases. It may even lead to the creation of tailored chemotherapy for each patient, as well as it may contribute to personalized care in other fields, and to help physicians identify the best course of treatment for patients. The research being conducted at the UHL and the UL is also receiving the collaboration of other facilities as the Cleveland Clinic and the Dana-Farber Institute/Harvard Cancer Center.
“These findings related to structure have provided fresh approaches to diseases such as intestinal cancer, inflammatory bowel diseases including ulcerative colitis, Crohn’s disease and diverticulosis. New mechanisms of cancer spread and progression as well as novel cellular targets have been identified,” Coffey said.
The researcher believes that the team is now able to better personalize operations to suit the exact stage of a patient’s disease, including Crohn’s, bowel cancer, and a range of abdominal conditions. “This has significant impact for patients as a more accurate understanding allows us opt for less invasive keyhole surgery with minimal blood loss, and, more importantly for the patient, minimal complications. With surgery that adopts the new mesenteric-based principles, previously common complications are now a rarity, patients recover quickly and achieve a normal quality of life faster, leading to savings in healthcare and socio-economic costs,” he explained.