In terms of physical disabilities, inflammatory bowel disease (IBD) falls into the “invisible” category. Most of the time, you can’t tell someone has IBD just by looking at them because a majority of the symptoms occur inside the body. Specifically, they occur in the intestines and other parts of the digestive tract.
However, a few symptoms occur in and on other parts of the body. The Crohn’s & Colitis Foundation reports that 5 percent of people with IBD suffer from skin disorders caused either from the disease itself or the medications used to treat it. I’m included in that group.
For most of my life, even before my Crohn’s diagnosis, I suffered off and on from atopic dermatitis and other skin rashes. At times, they became so bad that I risked getting a bacterial infection and had to take antibiotics along with topical and oral steroids to clear my skin. As if these persistent skin irritations weren’t bad enough, I started developing ulcers and open sores when my Crohn’s was at its most severe.
The ulcers in my mouth appeared first. I’m always biting my tongue or cheek when I eat, so I didn’t think much about them at first. But then I noticed that I was getting them more frequently, or even getting multiple ulcers at once. My gut pain was already taking a toll on my appetite, but the ulcers made eating downright excruciating. If the sores were on my cheeks, I could always chew my food on the other side of my mouth to avoid the stinging sensation. When the sores were on my tongue, there was no way I could prevent food or drink from touching the sensitive areas.
At least with the typical Crohn’s symptoms, I could force myself to eat and drink for nutrition’s sake when I didn’t have an appetite. But with the ulcers, I didn’t want anything in my mouth despite the hunger pangs. Some days I fought back tears just to get something in my stomach. I eventually discovered that by drinking through a straw, I could position it a certain way to avoid the ulcers. For weeks, I lived on Ensure and smoothies until the sores subsided or went away for a while.
While even the general population can empathize with the pain of mouth ulcers, not many can understand what I experienced when another, less common skin disorder manifested from my Crohn’s: pyoderma gangrenosum. Pyoderma gangrenosum is a skin ulcer that usually develops on the lower extremities. Mine erupted about five inches above my right inner ankle.
As I said, I’ve always been prone to dermatitis. Mosquitoes also love me, and I’m somewhat clumsy, so when a spot on my lower leg began to itch, I thought it was a rash, a bug bite, or a small scratch that had scabbed over. One day, I absentmindedly broke the skin with constant rubbing and scratching. I tried to avoid doing more damage and risking infection by putting a bandage over the area. After a few days, the area wasn’t healing but instead was growing larger. I graduated from the standard size bandage to the largest size bandage to keep the wound well covered and to prevent my pant leg from rubbing against it and making it worse.
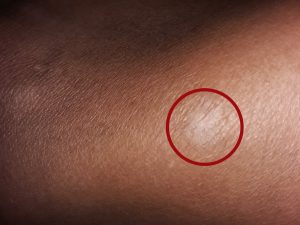
By that time, I had an appointment with my GI coming up, so I held off contacting him or going to my primary care physician because I’m stubborn and cheap. If you read my column last week about my high pain tolerance, I wasn’t going to allow a penny-sized crater in my leg kill me!
However, I did a Google search just to make sure my leg wasn’t going to turn black and get gangrene. Somehow, through my fairly accurate description of the red, open, weepy sore surrounded by yellowing, crusty skin, I found pictures of open wounds that looked exactly like mine, and the condition — pyoderma gangrenosum — was linked to IBD. I printed out the pictures and an article from my web search to bring to my doctor’s appointment, as if my GI wouldn’t know what I had. Nevertheless, I felt triumphant when he confirmed my suspicions.
Because I wasn’t responding to any of the medications I had been taking over the past two years, my GI decided to start me on Remicade (infliximab). He was confident that the infusions would help not just my internal symptoms, but also they would heal and prevent the mouth and skin ulcers, too. After my first infusion, the sores in my mouth and my leg began to heal almost immediately, and I haven’t had any issues with ulcers since. All that remains is a fading scar where the wound on my leg used to be.
***
Note: IBD News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of IBD News Today, or its parent company, BioNews Services, and are intended to spark discussion about issues pertaining to IBD.

