In part two of my four-part series about Crohn’s disease, I discuss the journey to a Crohn’s or colitis diagnosis. Crohn’s and colitis are both diseases that are not as simple to diagnose as other chronic illnesses.
 With Crohn’s or colitis, there’s no test that comes up positive for a treatment plan to begin. No, this disease cannot do anything “easily.” There is such a large number of signs and symptoms, and combinations of symptoms, that finding a diagnosis is not as simple as a yes or no answer.
With Crohn’s or colitis, there’s no test that comes up positive for a treatment plan to begin. No, this disease cannot do anything “easily.” There is such a large number of signs and symptoms, and combinations of symptoms, that finding a diagnosis is not as simple as a yes or no answer.
The first ‘go-to’ for getting your diagnosis is to see your primary care physician and say what’s going on. Your doctor will note your symptoms and other information you provide, and hopefully suggest a plan. I know bathroom talk is never pleasant, but it could save you future pain or risk of the disease spreading or getting worse with time.
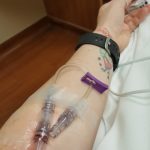
 Your primary doctor will usually recommend a referral for a consultation with a gastroenterologist if you have stomach issues. Then, after meeting with the GI, you’ll likely go through a colonoscopy, endoscopy, or both procedures so doctors can view your inflammation and take biopsies of what is seen. Blood work is usually ordered, such as a CBC (complete blood count), to look for anemia and infections; liver or kidney panels can be ordered, and typically at least one stool sample is requested.
Your primary doctor will usually recommend a referral for a consultation with a gastroenterologist if you have stomach issues. Then, after meeting with the GI, you’ll likely go through a colonoscopy, endoscopy, or both procedures so doctors can view your inflammation and take biopsies of what is seen. Blood work is usually ordered, such as a CBC (complete blood count), to look for anemia and infections; liver or kidney panels can be ordered, and typically at least one stool sample is requested.
A colonoscopy, coming up from the bottom, or an endoscopy, going down from the top, are scope procedures in which a tube is inserted into the body through the anus (up from the bottom) or mouth (down from the top) to look around. These are done under general anesthesia to help avoid any discomfort or embarrassment, and sometimes fasting is required as well as a bowel prep solution to drink (lots of it, too).
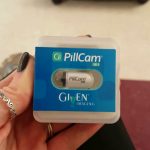 Sometimes a capsule endoscopy is used when neither an endoscopy nor colonoscopy spots site(s) of inflammation. In a capsule endoscopy, the patient swallows a large pill-sized camera and wears a receiver belt around the waist for the duration of the day. If all goes well, the belt is returned to the doctor’s office and the pill exits the body with normal waste, and your doctor views images much like a little documentary.
Sometimes a capsule endoscopy is used when neither an endoscopy nor colonoscopy spots site(s) of inflammation. In a capsule endoscopy, the patient swallows a large pill-sized camera and wears a receiver belt around the waist for the duration of the day. If all goes well, the belt is returned to the doctor’s office and the pill exits the body with normal waste, and your doctor views images much like a little documentary.
MRIs and CT scans, X-rays ‚ you get the picture — and blood work speaks for itself.
 With some patients, inflammation or ulcerations are found inside the stomach, bowel, colon, etc., and the doctors can easily take biopsies of these cobblestone-like features inside you. For some, there’s no pain and the disease is found by mere coincidence. Scopes and blood tests looking for inflammation lead to a diagnosis. For others, an obstruction or bowel blockage lands you in the ER, where doctors find that Crohn’s or colitis has thicken the bowel walls. Or, for others still, it takes a number of these things to finally get a diagnosis, like a sudden onset of a number of painful symptoms with no relief in sight. And then there’s those who are still searching for a diagnosis to the symptoms they have.
With some patients, inflammation or ulcerations are found inside the stomach, bowel, colon, etc., and the doctors can easily take biopsies of these cobblestone-like features inside you. For some, there’s no pain and the disease is found by mere coincidence. Scopes and blood tests looking for inflammation lead to a diagnosis. For others, an obstruction or bowel blockage lands you in the ER, where doctors find that Crohn’s or colitis has thicken the bowel walls. Or, for others still, it takes a number of these things to finally get a diagnosis, like a sudden onset of a number of painful symptoms with no relief in sight. And then there’s those who are still searching for a diagnosis to the symptoms they have.
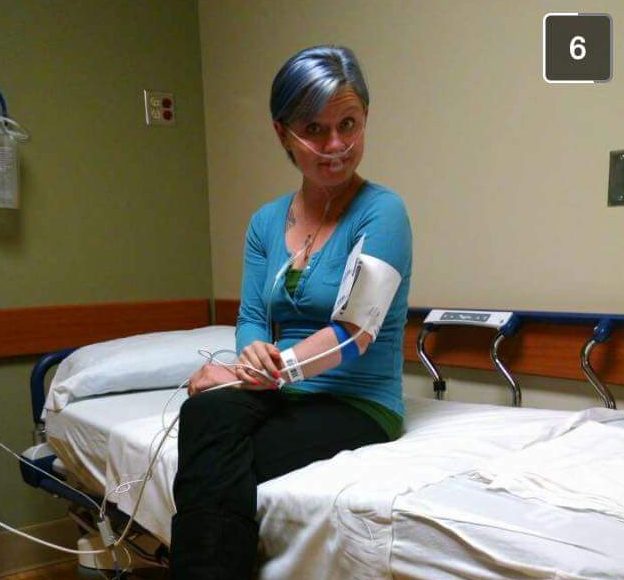 For me, a diagnosis took a little longer than two years. During those years, I underwent a number of colonoscopies, endoscopies, pill capsule endoscopies, CT scans and X-rays, doctor appointments and ER visits, and both of my bottom surgeries. (See Early Signs and Symptoms of My Crohn’s Disease and Welcome to ‘It Could Be Worse’).
For me, a diagnosis took a little longer than two years. During those years, I underwent a number of colonoscopies, endoscopies, pill capsule endoscopies, CT scans and X-rays, doctor appointments and ER visits, and both of my bottom surgeries. (See Early Signs and Symptoms of My Crohn’s Disease and Welcome to ‘It Could Be Worse’).
I cannot diagnose or provide treatment suggestions, but I would only recommend highly that you see your doctor if you are having problems you think might be Crohn’s or colitis before these problems get worse. Because, it could be worse.
Note: IBD News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of IBD News Today, or its parent company, BioNews Services, and are intended to spark discussion about issues pertaining to inflammatory bowel disease.

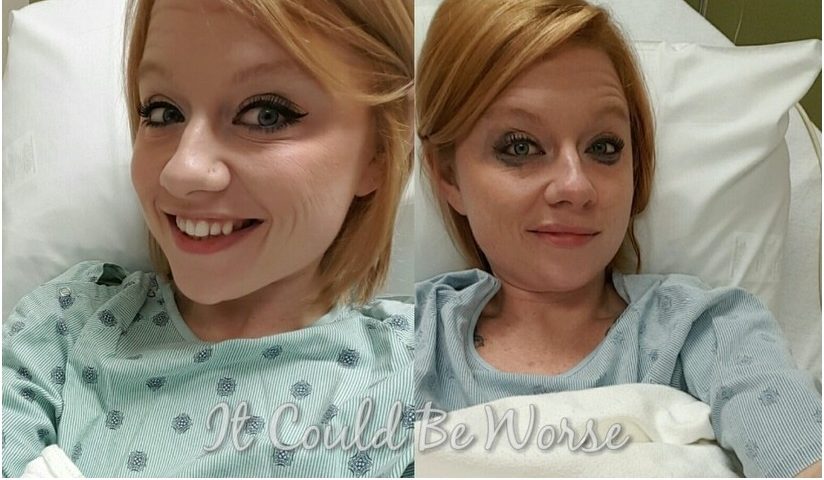
Where do they do scopes under general anesthesia?! Herein Canada it’s “sedation” but I can vividly remember what my intestines looked like on the screen the doctors had in the room and I was crying due to the pain. I was diagnosed with UC, had full collectomy after losing 40lbs in a month (105lbs to 65!) After 6 months in the hospital, 2 more surgeries, recovering and thinking I was done with the horror, I got sick again and boom. Crohns. People see me and they see my well practiced smile and have no idea the hell going on inside my body and as a result, my mind. I don’t know what my point is but I do seem to be less sick when I’m thriving in life. Doing well now but there’s always the heaviness of impending doom.
Here, the sedation is anesthesia, but conscious sedation, so the patient can easily be woken up. However, I did wake up during my first scope, I was crying in pain as they moved around my bowel. I saw mine on the screen as well. I truly hope you have found some relief! And I wish you luck. Just keep your head up, it is truly hard to show the inside pain while keeping a smile. *Hugs*
I have to be under anesthesia, as my colrectal surgeon says ask for the milk of anesthesia, it is Propofol.Versed,demorol none of those work for me. I always have to go to a hospital to have a colonoscopy or endoscopy because the outpatient endoscopy places can’t give what I need. the pain is not tolerable if I’m not knocked out, plus with having 7 resections I have alot of kinks and places hard to maneuver. I say I don’t want to feel it and I’ll do it.